Diabetic Retinopathy
Introduction to Diabetic Retinopathy (DR)
According to the American Academy of Ophthalmology, more than 4.4 million people in the United States over the age of 40 suffer from diabetic retinopathy, or DR. The Academy recommends regular screening for retinopathy in all patients with diabetes.
Background Diabetic Retinopathy
Early manifestations of DR include microscopic spots of bleeding in and around the fovea, which is the center of the retina responsible for good vision. In poorly controlled diabetes, the severity of retinal bleeding worsens with time. If background DR is left untreated, it can progress to proliferative DR and eventually permanent vision loss.
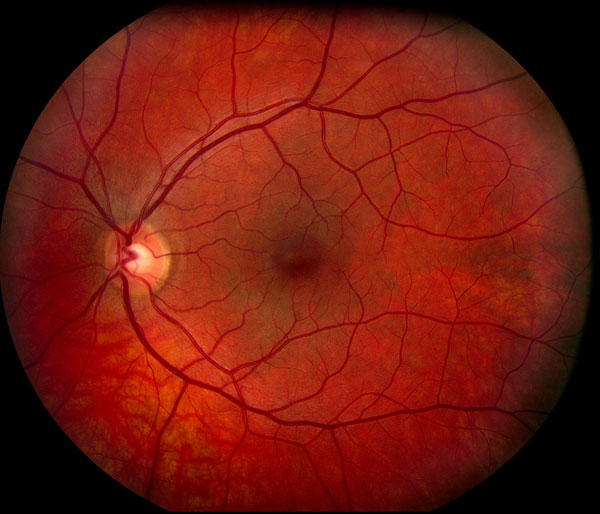
Normal Retina: Note the fovea (the dark red spot in the center), the healthy pink retinal color, and normal blood vessels surrounding it without any bleeding.
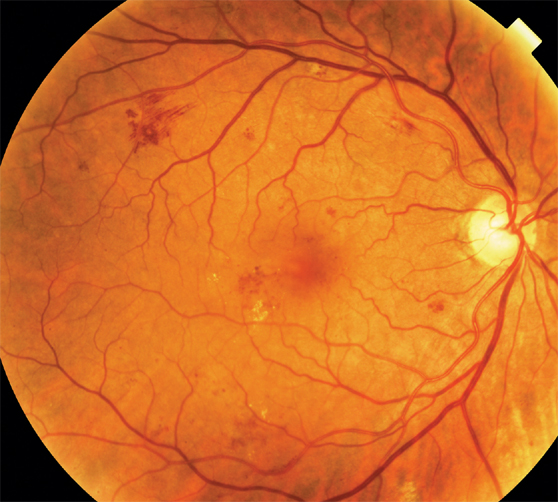
Background Diabetic Retinopathy: Note the red spots of bleeding and yellow spots of cholesterol leakage throughout the retina. Compare this to a picture of a normal retina (see picture on right).
Proliferative Diabetic Retinopathy
Proliferative DR results from severe retinal bleeding due to uncontrolled diabetes, leading to severe loss of vision, retinal scarring, and vision-threatening retinal detachments. Some of these complications require surgical treatment, but despite surgical intervention some patients unfortunately develop irreversible vision loss. The goal of annual screening is to prevent this devastating sequela of diabetic retinopathy.
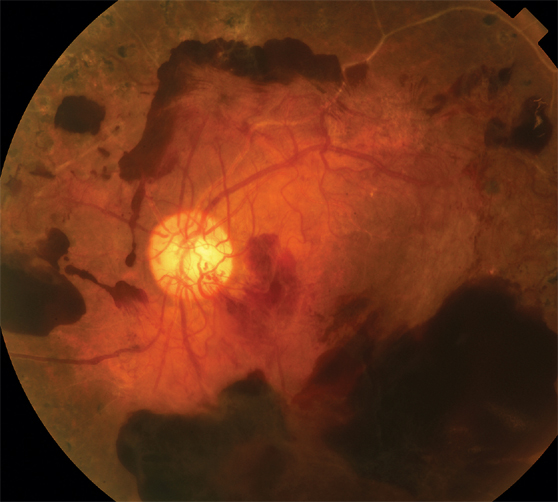
Picture of proliferative DR; note the active bleeding (dark red blots) in the retina and the formation of abnormal, leaky blood vessels over the optic nerve (the yellow disc in the middle of the photograph).
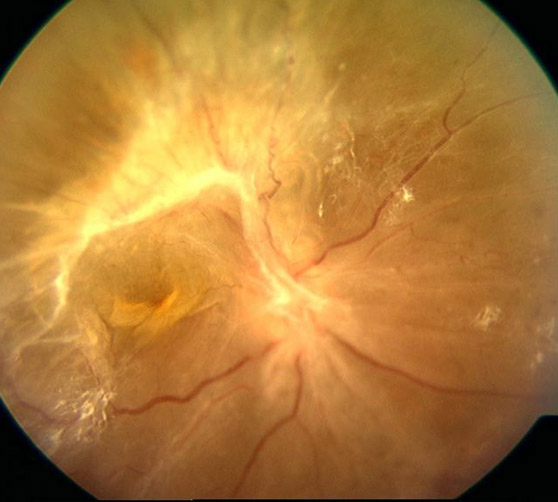
Picture of tractional retinal detachment from severe DR. Note the severe white scarring within the retina, the distorted architecture of the retinal blood vessels, and the loss of the healthy pink color of the retina.
Diabetic Macular Edema (DME)
Macular edema is defined as swelling of the fovea at the center of the retina. High blood glucose from poorly controlled diabetes causes the retinal blood vessels to leak fluid, which seeps into the surrounding retinal tissue, causing swelling. Swelling of the retina compromises one’s vision, since the healthy retina is normally thin and “dry.” Macular edema can occur at ANY stage of diabetic retinopathy, and may or may not accompany retinal bleeding. Some patients may notice decreased vision or distortion in their central vision, but others may have no symptoms at all from DME. Therefore, it is crucial to undergo regular screening eye exams in order to diagnose and treatment macular edema.
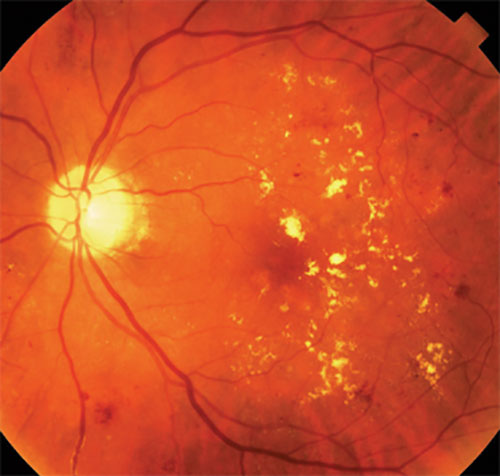
Picture of diabetic macular edema; note the yellow cholesterol deposits from abnormal fluid leakage towards the center of the retina (the dark red spot in the middle of the photograph).
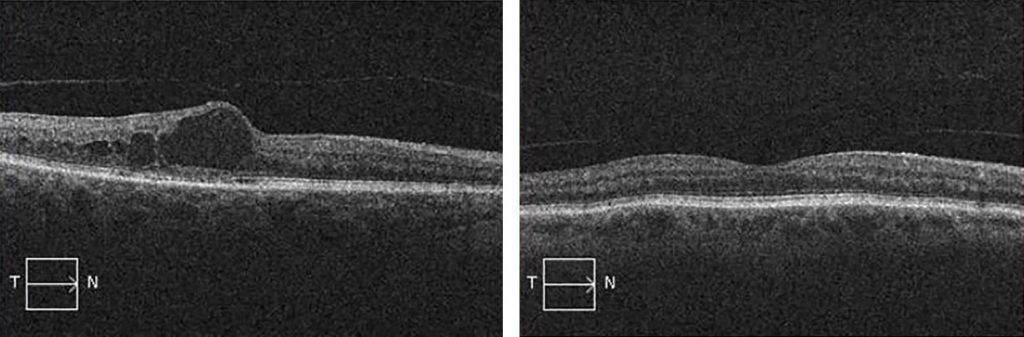
OCT image of diabetic macular edema (LEFT image). Note the large cystic structure filled with fluid (represented by the dark void) within the retinal tissue in the center of the image, which represents swelling at the fovea. Contrast this with a normal appearing retina (RIGHT image), where the tissue is uniformly thin without swelling at the fovea.
Why does my vision fluctuate when my blood sugar is high or low?
One thing a patient with poorly controlled diabetes who also wears glasses may notice is that her vision may fluctuate with her blood glucose level. When a person’s blood glucose is exceptionally high or low, her glasses prescription may change drastically. When the glucose level returns to normal, so too does the power in the glasses prescription. Therefore, we do not recommend that patients fill their glasses prescription based on a refraction (i.e. a glasses check) performed in clinic during a time when their blood glucose is very high or very low.
